WATCHMAN: A one-time implant that helps reduce AFib stroke risk
Dignity Health – Memorial Hospital offers patients with non-valvular atrial fibrillation (also called AFib or AF) an alternative to long-term warfarin medication with the WATCHMAN™ Left Atrial Appendage Closure (LAAC) Implant.
How does AFib increase stroke risk?
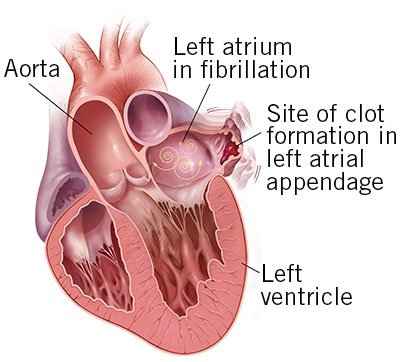
The average person with atrial fibrillation (also called AFib or AF) is five times more likely to have a stroke than someone with a regular heartbeat. That’s because AFib can decrease the heart’s pumping capacity by as much as 30%. Since blood isn’t pumped out of the heart normally, it’s easier for blood cells to stick together and form clots in an area of the heart called the left atrial appendage (LAA). When a blood clot escapes from the LAA and travels to another part of the body, it can cut off the blood supply to the brain, causing a stroke.
In people with atrial fibrillation not caused by heart valve problems (the most common type of AFib), more than 90% of stroke-causing clots that come from the heart are formed in the LAA.
Reducing AFib stroke risk
 Blood thinners, also called anticoagulants, are an effective way to lower the risk of stroke in people with atrial fibrillation not caused by heart valve problems. Common blood thinners include warfarin, also known as Coumadin®, Eliquis®, Pradaxa®, Xarelto®, and Savaysa®.
Blood thinners, also called anticoagulants, are an effective way to lower the risk of stroke in people with atrial fibrillation not caused by heart valve problems. Common blood thinners include warfarin, also known as Coumadin®, Eliquis®, Pradaxa®, Xarelto®, and Savaysa®.
But some people need an alternative to blood thinners, because they can increase the risk of bleeding. Some bleeding events are minor and easily treated, like a cut taking longer than normal to stop bleeding. In other cases, the bleeding can be life-threatening, such as when bleeding in the brain causes a stroke.
If you have a history of bleeding or a lifestyle, occupation, or condition that puts you at risk for bleeding, your doctor may consider an alternative to blood thinners, such as the WATCHMAN Implant.
An alternative to blood thinners
WATCHMAN is a permanent implant that offers an alternative to the lifelong use of blood thinners. It’s about the size of a quarter and is made from very light and compact materials commonly used in many other medical implants.
How WATCHMAN works
WATCHMAN effectively reduces the risk of stroke by permanently closing off the LAA to keep blood clots from escaping. WATCHMAN can eliminate the bleeding risks and regular blood tests and food-and-drink restrictions that come with warfarin. In a clinical trial, 9 out of 10 people were able to stop taking warfarin just 45 days after the WATCHMAN procedure.
How is WATCHMAN implanted?
WATCHMAN is implanted into your heart in a one-time procedure. To implant WATCHMAN, your doctor makes a small cut in your upper leg and inserts a narrow tube, as done in a standard stent procedure. Your doctor then guides WATCHMAN into your heart’s LAA. The procedure is done under general anesthesia and takes about an hour. Patients commonly stay in the hospital overnight and leave the next day.
After the procedure
Following the WATCHMAN procedure, you’ll take warfarin for 45 days or until your LAA is permanently closed off. During this time, heart tissue will grow over the implant to form a barrier against blood clots. Your doctor will monitor this process by taking pictures of your heart to see when you can stop taking warfarin.
Your doctor will then prescribe a medicine called clopidogrel (also known as Plavix®) and aspirin for you to take for six months. After that, you’ll continue to take aspirin on an ongoing basis. A very small number of patients may need to keep taking blood thinners long term.
In a clinical trial:
- 92% of patients were able to stop taking warfarin just 45 days after the procedure
- 99% of patients were able to stop taking warfarin within 1 year after the procedure
Is WATCHMAN right for you?
If you have a history of bleeding or a lifestyle, occupation, or condition that puts you at risk for bleeding, WATCHMAN may be right for you. But like any medical procedure, WATCHMAN comes with risks, so it isn’t right for everyone. Your cardiologist will weigh your risk of a stroke against your risk of a serious bleeding problem to determine the right treatment for you.
Learn more
Talk to your physician to determine if WATCHMAN is right for you. To find a doctor, please call (661) 324-7070 or use our online Find a Doctor tool.


 Blood thinners, also called anticoagulants, are an effective way to lower the risk of stroke in people with atrial fibrillation not caused by heart valve problems. Common blood thinners include warfarin, also known as Coumadin®, Eliquis®, Pradaxa®, Xarelto®, and Savaysa®.
Blood thinners, also called anticoagulants, are an effective way to lower the risk of stroke in people with atrial fibrillation not caused by heart valve problems. Common blood thinners include warfarin, also known as Coumadin®, Eliquis®, Pradaxa®, Xarelto®, and Savaysa®.