The Dignity Health website is moving to CommonSpirit.org to deliver a more patient-centered digital experience across CA, AZ, and NV.
Exciting changes are coming!
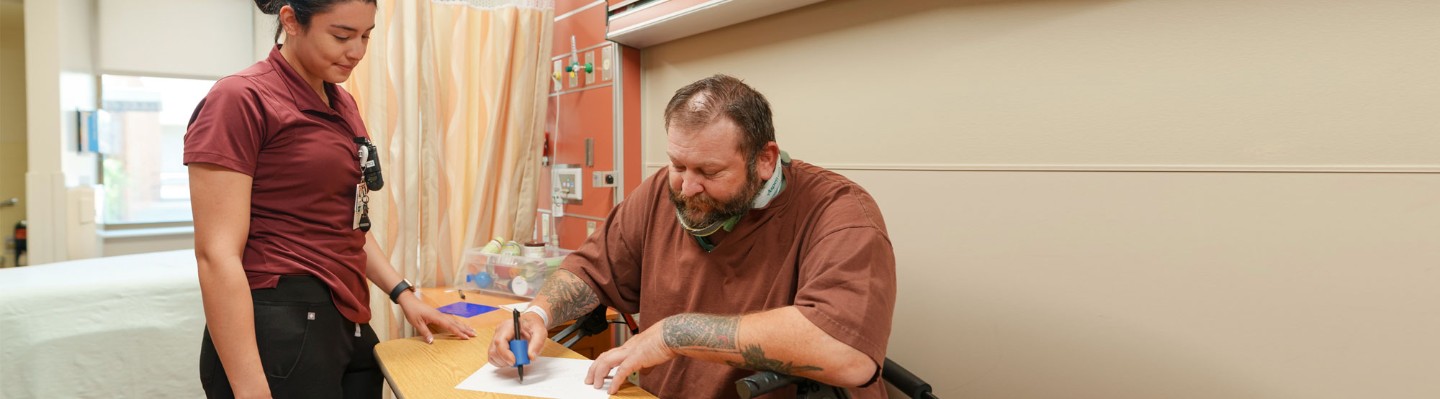
Patients differ in severity of impairment and limitations in function. Therefore, the length of stay for rehabilitation varies based on medical condition, goals of the patient, progress and a number of other factors. Generally, the length of stay averages 7-14 days. Your care coordinator will be able to give you an estimated length of stay for your particular situation and update you as you progress through your rehabilitation program
Visiting hours are preferably between 4 to 8 p.m. because the majority of the day is filled with therapeutic activities. Visitors are an important part of the rehabilitation process and are welcome to observe therapy as long as it doesn’t interfere with treatment and patient progress. Please note that upon arrival, all visitors must go to the main hospital entrance to obtain a visitor’s badge.
With few exceptions, patients require assistance and/or supervision from their family or caregiver once they are discharged from the Acute Rehabilitation Program. For this reason, family/caregivers actively participate in multiple education and training sessions throughout the patient's stay. Interpreters are available upon request.
Outside food and beverages must be cleared with your nurse to ensure your safety and health. Your physician, nurse and speech therapist will evaluate your swallowing capabilities and advise on any dietary restrictions you might have.
Please bring personal items and clothing with you for your stay on the Inpatient Rehabilitation Unit. Laundry services are not provided, so please arrange with your family or caregiver to wash your clothing. We do not recommend that you bring any valuable items such as cash, jewelry or electronics (laptops, tablets, etc.). You can bring your cell phone, but we are not responsible for any lost or damaged items. We do have a computer available for patients and family members. There is no need for money, jewelry or credit cards while you are in the IRU.
List of items to bring:
Overall safety and the well-being of our patients are essential parts of our care and philosophy in the Inpatient Rehabilitation Unit at Mercy General Hospital. The following are recommendations to ensure you and your family/caregiver remain safe while on the unit.
Do not leave the unit without talking to your nurse first. Call lights are available in each room and restroom. Use these call lights anytime you need assistance. There may be a fire drill during your stay. In that event, please follow staff instructions through the process. This facility is a non-smoking facility.
Most rehabilitation patients are discharged to the community setting, either home with family and caregivers, to a board and care facility or an assisted living facility. You should plan to have some level of assistance when you return home. Occasionally, a patient will be discharged to a skilled nursing facility or another acute care hospital.
Discharge planning starts before admission and continues throughout your stay. Your discharge destination is determined by many factors including, but not limited to, your support system, insurance coverage, progress and level of assistance needed. You, your family and friends, and the Inpatient Rehabilitation Unit (IRU) team are all involved in your discharge planning. We will make all the necessary arrangements for equipment and therapy after discharge. Medications will be called into your pharmacy 24 hours before discharge whenever possible, or you can ask your nurse about how they can be delivered to your room on the day of discharge. Preferred discharge time is 11 a.m. Arrangement for continued post-hospital services will be made for you.
You will be contacted after discharge to follow up on your treatment. You may receive follow-up calls to check on your progress starting within 3 days and continuing up to 3 months post discharge. We want to ensure you are continuing to progress and offer any assistance we can.
You may also receive a patient satisfaction survey asking about your experience on the IRU. If you have any questions or concerns with your care during or after discharge, please call the Program Director at (916) 453-4689 and share your concerns. We want to do everything we can to make your stay here as positive as possible.